Understanding Necrosis: Causes, Types, and Treatment
Learn the basics of necrosis, necrotic tissue, and common treatment methods.
Published on March 20, 2024. Reviewed by Tara Call Triplett RN, WCC, CHFN
Necrosis: Definition and overview
Necrosis, a term derived from the Greek word "nekros" meaning "dead," is a type of cell damage that leads to the premature death of cells in living tissue by autolysis, the breakdown of cells by the body’s own enzymes. Necrosis is a process involved in various conditions ranging from infections to cancers, fundamentally affecting the tissue's structure and function.
Unlike apoptosis, a programmed and orderly cell death, necrosis is often considered unregulated or chaotic and can lead to detrimental inflammation in the surrounding tissue. Tissue death occurs when there is not enough blood flow available to the tissue.
Necrosis, without proper management and treatment, can have life-threatening impacts for patients. By understanding necrosis, the different types, and the underlying causes, wound care clinicians can deliver more personalized treatment that promotes healing, reduces infection, and enhances patients’ quality of life.
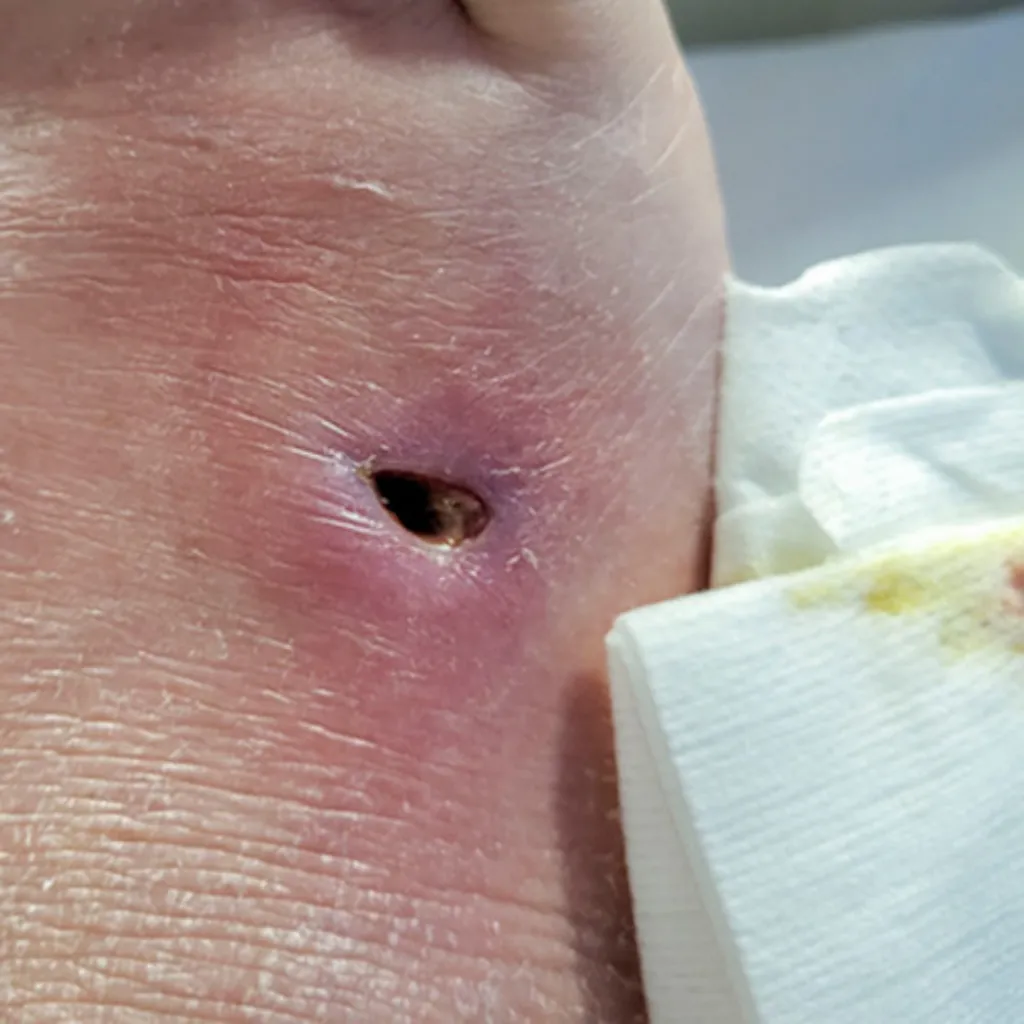
What is necrosis?
Necrosis is depicted by a sequence of morphological changes, including cell swelling, membrane rupture, and the breakdown of organelle. The process leads to the release of cellular contents into the surrounding tissue, triggering an inflammatory response that can cause further tissue damage.
Necrosis can affect any tissue in the body and is associated with a variety of conditions including infections, injuries, and ischemic conditions where blood flow to the tissue and bone is obstructed.
What is necrotic tissue?
Necrotic tissue refers to the dead or dying cells and tissues resulting from necrosis. This tissue is no longer viable and cannot carry out its normal functions. It may appear discolored, swollen, and may have a foul odor. We dive deeper into the details of necrotic tissue in our full blog below.
Types of necrosis:
There are several types of necrosis, each with specific characteristics depending on the affected tissue and the underlying cause. These include:
1. Coagulative necrosis: This typically results from a lack of blood supply (ischemia) to an organ, especially the heart.
2. Liquefactive necrosis: Often occurring in the brain, this involves the transformation of the tissue into a liquid viscous mass.
3. Caseous necrosis: This is a form of necrosis in which the tissue acquires a cheese-like appearance, commonly associated with tuberculosis.
4. Fat necrosis: This necrosis type is when fat tissue is broken down into fatty acids in the presence of certain enzymes.
5. Gangrenous necrosis: Since this necrosis type is a term for ischemic necrosis of the limb, it falls in the same category as coagulative necrosis. Being one of the more common necrosis types in wound care, it presents as either dry gangrene or wet gangrene, or ischemia with a bacterial infection. Wet gangrene leads to liquefactive necrosis of the tissues.
6. Fibrinoid necrosis: This necrosis involves immune complexes and fibrin deposition in the walls of blood vessels.
Other Types of Necrosis
- Acute Tubular Necrosis - Acute tubular necrosis is a condition characterized by the damage and death of the tubular cells in the kidneys. ATN is often caused by a lack of blood flow (ischemia) or exposure to nephrotoxic agents that directly harm the kidney cells.
- Uvular Necrosis - The uvula is noted as the small, fleshy extension at the back of the soft palate that hangs above the throat. Uvular necrosis refers to the death of the uvular tissue. This condition can result from mechanical interruption of the blood supply to the uvula.
How to treat necrosis
Treatment for necrosis depends on its cause, location, and extent. General strategies include removing the source of injury, preserving viable tissue, and managing pain. Specific treatments may involve:
- Surgical intervention such as debridement to remove dead tissue, or in cases of avascular necrosis, procedures like bone grafts, osteotomy (cutting and realigning bones), or joint replacement.
- Medications to treat any underlying condition or to manage pain.
- Breathing pure oxygen in a pressurized room to enhance the body's natural healing processes can be used for certain types of necrosis.
Want to learn more about necrosis and how to treat necrotic tissue?
Our Skin and Wound Management courses help you advance your clinical knowledge on providing effective wound care treatment. Prepare for the NAWCO® credentialing exam with our online or onsite course options.