Necrotic Tissue: Understanding the Basics & Treatment Options:
We dive into the fundamentals of necrotic tissue, common causes, and treatment options.
Published on March 20, 2024. Reviewed by Tara Call Triplett RN, WCC, CHFN
So, what is necrotic tissue?
Necrotic tissue refers to the dead or dying cells and tissues resulting from necrosis. This tissue is no longer viable and cannot carry out its normal functions. It may appear discolored, swollen, and may have a foul odor due to the release of cellular debris and toxins. Identifying necrotic tissue in wounds helps wound care clinicians provide appropriate care.
Necrotic tissue must be removed to prevent the spread of infection and promote healing. This can be achieved through debridement or other interventions aimed at removing the dead tissue while preserving healthy surrounding tissue. Understanding the causes, types, characteristics, and treatment options for necrotic tissue is crucial for effective management and prevention of complications.
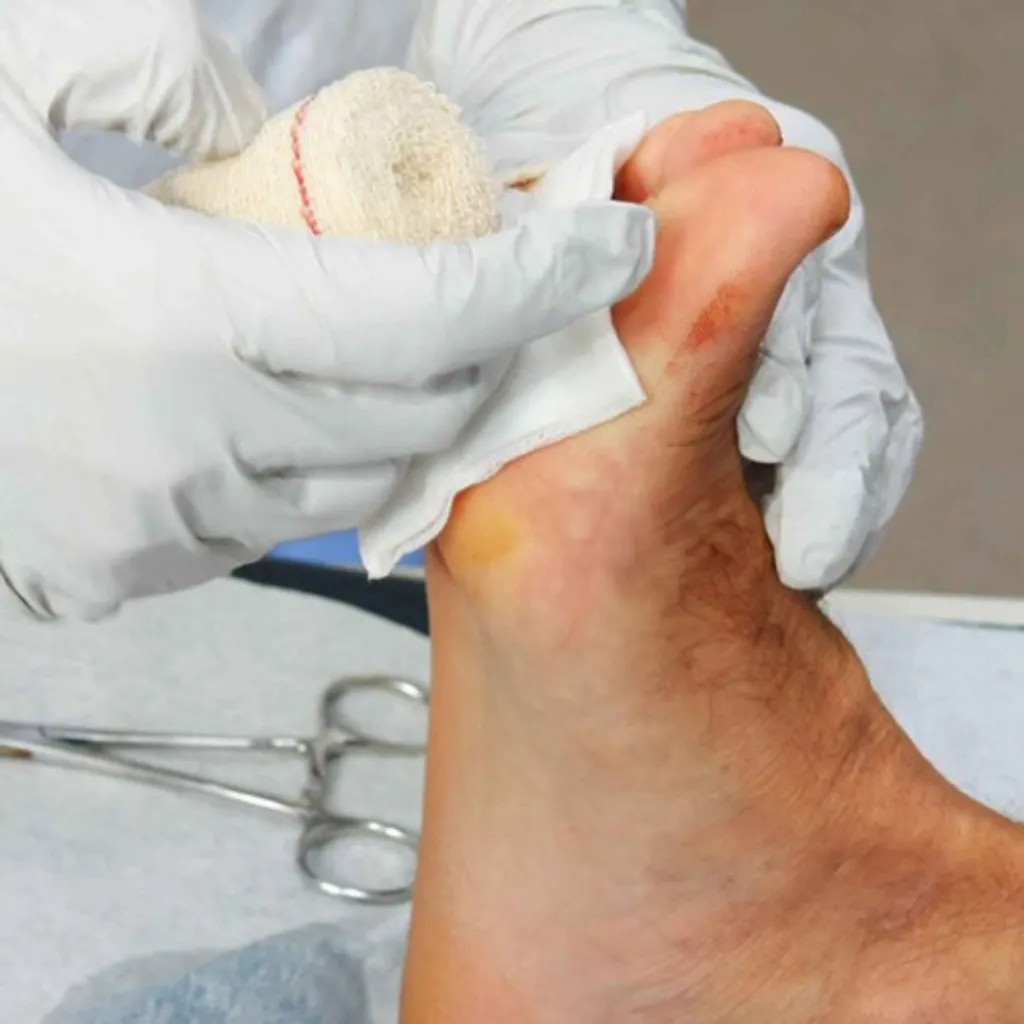
Causes of necrotic tissue
Recognizing underlying causes of necrotic tissue allows clinicians to intervene earlier and prevent further wound deterioration. Several factors can contribute to the development of necrotic tissue, including:
1. Ischemia
Lack of blood flow to a particular area can lead to tissue death due to inadequate oxygen and nutrient supply. Ischemic necrosis commonly occurs in conditions such as heart attacks, strokes, and peripheral artery disease.
2. Infection
Bacterial, viral, or fungal infections can cause tissue necrosis by triggering an inflammatory response that damages cells and impairs blood flow. Conditions like gangrene, necrotizing fasciitis, and sepsis are examples of infections that can result in necrotic tissue.
3. Trauma
Physical injuries, burns, frostbite, and surgical procedures can cause direct damage to tissues, leading to cell death and necrosis.
4. Toxins
Exposure to toxins from chemicals, drugs, or venomous substances can induce cellular damage and necrosis. Examples include carbon monoxide poisoning, drug-induced liver injury, and venomous snake bites.
5. Underlying medical conditions
Certain medical conditions such as diabetes, autoimmune diseases, and cancer can predispose individuals to necrotic tissue formation due to impaired circulation, compromised immune function, or tumor-related necrosis.
Types of necrotic tissue:
Necrotic tissue can present in various forms, each with distinct characteristics:
Dry necrosis
Also known as coagulative necrosis, this type typically occurs in solid organs like the heart, kidney, or liver. It is characterized by the preservation of tissue architecture with a dry, firm appearance due to protein denaturation. Dry necrosis often results from ischemic events and may be noted on distal extremities, such as ankles, toes, and fingers. It is often black or dark brown in color and coarse or leathery in texture. This is often referred to as dry gangrene and is often seen in patients with peripheral arterial disease.
Wet necrosis
Also referred to as liquefactive necrosis, this type is characterized by the rapid dissolution of necrotic tissue, leading to the formation of fluid-filled cavities. It is commonly seen in infections, particularly bacterial and fungal, where the inflammatory response results in tissue liquefaction.
This is often referred to as wet gangrene, and diabetic patients are especially susceptible due to hyperglycemia and infections of diabetic foot wounds. Bacterial infections can result in gas production causing a rapid spread of infection and tissue necrosis and should be treated upon detection.Caseous necrosis
This form of necrosis is characterized by a cheese-like, crumbly appearance of the affected tissue. It is often associated with granulomatous infections such as tuberculosis, where immune cells wall off the infected area, leading to central necrosis.
Fat necrosis
Fat necrosis occurs when adipose tissue undergoes necrosis, typically due to trauma or inflammation. It can present as palpable nodules or areas of firmness in the affected fatty tissue.
Common characteristics:
The characteristics of necrotic tissue vary depending on the underlying cause, location, and extent of tissue involvement. However, common signs and symptoms may include:
- Pain: Necrotic tissue can be associated with localized or diffuse pain, which may range from mild discomfort to severe to debilitating.
- Swelling: Inflammation and fluid accumulation in the affected area can lead to swelling, redness, and warmth.
- Discoloration: Necrotic tissue often appears darker or discolored, ranging from pale white or yellowish (slough) to dark brown or black (eschar). Slough may be adherent to the wound bed or nonadherent. Eschar is typically well adhered to the wound bed.
- Odor: In cases of wet necrosis or gangrene, the presence of bacteria and tissue breakdown can result in a foul odor emanating from the affected area.
- Systemic symptoms: Severe cases of necrotic tissue, especially those associated with infections or underlying medical conditions, may present with systemic symptoms such as fever, chills, fatigue, and malaise.
Treatment options for necrotic tissue:
For all wound care professionals, the goals for treating necrotic tissue are to remove dead tissue, promote healing, and address the underlying cause. For a more detailed look at treating necrotic tissue, check out our full necrosis blog write-up.
Understanding and practicing effective treatment methods helps clinicians reach better patient outcomes. Treatment options may include:
1. Debridement:
Surgical debridement or enzymatic debridement using specialized dressings may be necessary to remove necrotic tissue and promote wound healing. Other options include autolytic, mechanical, enzymatic, and biologic debridement.
2. Antibiotics:
In cases of infection-related necrosis, antibiotics or antifungal medications may be prescribed to control the underlying infection and prevent further tissue damage.
3. Wound care:
Proper wound care, including cleaning, dressing changes, and wound protection, is essential for preventing complications and promoting tissue regeneration.
4. Revascularization:
In ischemic necrosis where blood flow to tissue and bone is lost, procedures such as angioplasty, bypass surgery, or thrombolytic therapy may be performed to restore the blood supply to the affected area and salvage viable tissue.
5. Pain management:
Analgesic medications may be prescribed to alleviate pain associated with necrotic tissue and improve the patient's comfort.
6. Underlying condition management:
Treating underlying medical conditions such as diabetes, autoimmune diseases, or vascular disorders is crucial for preventing recurrent episodes of necrosis.
7. Hyperbaric oxygen:
This method may be used as an adjunct treatment for specific conditions such as treatment of Wagner grade 3 or greater diabetic wounds of the lower extremity. These wounds typically have some degree of necrotic tissue.
Necrotic tissue is a serious medical condition. Recognizing the symptoms, understanding the different types of necrotic tissue, and implementing appropriate treatment strategies are essential for optimizing patient outcomes and preventing complications.
Early intervention and comprehensive wound care are key components of managing necrotic tissue and promoting tissue healing and regeneration.
By looking more closely at necrosis, wound care clinicians are better equipped to recognize it, begin early treatment, and help educate patients and their caregivers to ensure better outcomes.
Want to learn how to treat necrotic tissue and other skin wounds?
Our Skin and Wound Management courses help you advance your clinical knowledge on providing effective wound care treatment. Prepare for the NAWCO® credentialing exam with our online or onsite course options.